Slide Show - Understanding MDS-related Anemia
This slide show provides an overview of myelodysplastic syndromes (MDS) and MDS-related anemia, including the causes, common symptoms, and diagnosis. It also describes the different types of MDS, risk scores, and explains that the disease can range in its severity.
Click here to take our SURVEY
Your feedback is important to us! We will use your feedback to develop future areas of content about MDS which will help other patients, caregivers and families.
Animation - Understanding MDS-related Anemia
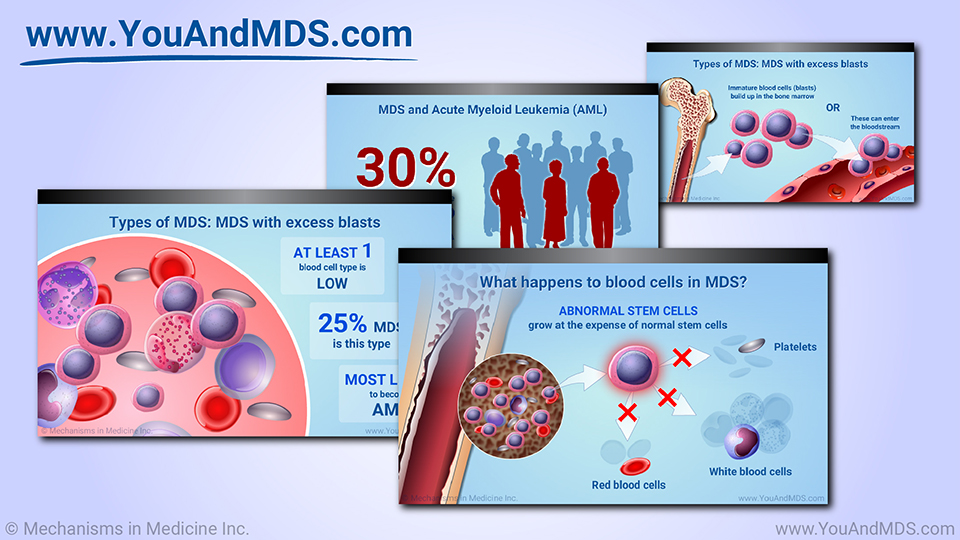
Slide Show - Understanding MDS-related Anemia

1.
What is MDS-related anemia? What causes it?

2.
What is a complete blood count? How does it show if I have anemia?

3.
What are the symptoms of MDS-related anemia?

4.
What makes people with MDS more likely to have anemia?

5.
What happens in MDS-related anemia over time?

6.
What’s the prognosis for MDS-related anemia? How is prognosis determined?

7.
Which questions should I ask my doctor about my MDS-related anemia?

8.
How is MDS-related anemia diagnosed?

9.
How is MDS-related anemia screened and monitored?

10.
Which other conditions have symptoms similar to MDS-related anemia?

11.
If I have MDS-related anemia, what should I watch out for in daily life?

12.
Which specific diagnosis questions should I ask my doctor about my MDS?

13.
How does acute myeloid leukemia (AML) relate to MDS?

14.
Why is it important to understand the causes of unexplained anemia?

15.
Abby’s story: How did you find out you had MDS-related Anemia?

16.
Barry’s story: How did you find out you had MDS-related Anemia?

17.
Bill’s story: How did you find out you had MDS-related Anemia?

18.
Abby’s story: How was your MDS-related Anemia diagnosed?

19.
Barry’s story: How was your MDS-related Anemia diagnosed?

20.
Bill’s story: How was your MDS-related Anemia diagnosed?